Midwifery Lead Unit (MLU) - Eden Suite
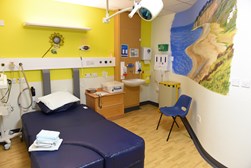


Eden Suite has five home-from-home rooms, two of which have birthing pools for water births.
Eden Suite is a home from home midwifery-led birthing unit at Arrowe Park Hospital that offers a welcoming, safe and relaxed environment. The suite is staffed by experienced midwives who are passionate about promoting natural labour and normal birth.
Why choose to have your baby on Eden Suite?
Giving birth is generally very safe. Evidence suggests that healthy women with uncomplicated pregnancies who plan to give birth in an alongside midwifery-led unit having fewer interventions during labour, for example to drip to speed labour up, and are less likely to need forceps or have a caesarean section. They have significantly more normal births than women who give birth in an obstetric unit with no difference in outcome for the baby.
Butterfly suite


The Maternity Ward
Some women need care in hospital during the antenatal period and most women come to the Maternity Ward after they have had their baby unless they have been discharged from Delivery Suite or Eden Suite. Care is provided on the Maternity Ward on the first floor of the Wirral Women and Children’s Hospital.
We hope this information on the website is helpful to you during your stay. You can also download our Maternity Ward Folder with detailed information about your stay using this link Maternity Ward Folder
Our Maternity Ward has:
Side Rooms
There are 26 side rooms on the ward.
Each side room has its own bathroom with a shower, toilet, and sink.
Post-Theatre Recovery Bay
The recovery bay has 6 beds.
This area has a bathroom for patients.
Please Note: Birthing partners must use the visitor's toilet located just off the maternity ward.
Baby Clinic Room
This is where the new born examination takes place.
Milk Room
The milk room is for staff use.
There is a freezer for storing frozen breast milk and a fridge for storing formula or expressed breast milk.
Items must be labelled, and we can provide the labels.
Transitional Care
The Postnatal ward also has four “Transitional Care” rooms that are used when babies require additional support that can be provided outside the Neonatal Unit.
Visitors
We warmly welcome your chosen birthing partner at all times and they can stay overnight to help you with your baby if you want.
- Your new-born's siblings can visit any time during the day time.
- Only children that are siblings of the new born baby can visit.
- Additionally, two other visitors (adults over 18 years) are allowed at a time.
Visiting hours are between 1PM-3PM and 6PM-7PM.
Please Note: Visitors must not use the toilet or wash facilities in the patients room or recovery bay. Visitors must use the toilets located just off the maternity ward.
Meal Times
Breakfast: 7:30-8:30 AM
We have a buffet breakfast with cereals, toast, jams, and marmalade. You can find this in the main corridor and use the toaster in the patient kitchen. There is also a microwave you can use. If you need to use the patient fridge, please label your food with your name and date. Your support partner can also use the breakfast facilities.
Lunch: 12:00-12:30 PM
Lunch is served in the main corridor. You or your support partner can collect your meal, but staff can help if you need it.
Dinner: 5:00 PM
Dinner is served in the main corridor with a selection of menu choices available at the meal trolley.
Please Note: We cannot provide lunch or dinner for birthing partners
Please inform a member of the team if you have any allergies or special dietary requirements
Refreshments
Drinks
Water fountains are around the ward. Please help yourself, but do not fill
water bottles directly from the fountain for hygiene reasons. The tea and
coffee machine is in the main corridor and available at any time.
Fridge
A fridge is located on the main corridor next to the hot drinks trolley
where food items can be stored.
Please Note:
Food stored in the fridge must have a sticker with persons
name along with the date and time the food was put in the fridge.
Snacks
There are vending machines with snacks and drinks on the ground floor corridor. They are accessible
24 hours a day (managed by external companies).
Delivery Suite/Labour Ward
The delivery suite is where anyone who isn’t low risk will be give birth, this is also where care is given to ladies who have additional risk factors and requiring additional care in the antenatal, intrapartum or postnatal period.
Who has risk factors? - Anyone who is being induced, less than 37 weeks pregnant, has a high risk obstetric or medical condition, unwell or with a fetal well-being concern.
We have:
- 8 Delivery rooms – 7 are ensuite
- High risk pool room (suitable for women who meet a criteria based on safety recommendations & availability)
- 2 High Dependency rooms
- Emergency maternity theatre and recovery room
- Bereavement suite
- Level 3 Neonatal Unit in immediate vicinity
- There are two designated Maternity Theatres directly linked to the Delivery Suite and MLU which are staffed 24 hours per day for elective and emergency surgery
- A designated Induction of Labour Suite based within our Delivery Suite - this is a 3 bedded area with shared bathroom facilities. Each space has 3 walls and a curtain for privacy.
This is one of our Delivery Rooms which has ensuite facilities. We have Delivery Beds that can be used in a variety of positions to support you using different positions in labour, mood lighting, music players, monitoring equipment to monitor you and your baby and a resuscitare for if your baby needs any support when they are born.

This is a photo of our high risk birthing pool which is based in one of our High Dependency Rooms on Delivery Suite. If you have risk factors depending on what they are it may still be suitable for you to use the birth pool. It may be recommended if you are recommended to have continuous monitoring of your babies heart beat or if you are being induced. Depending on your risk factors you may be recommended to get out of the birth pool when you are giving birth but can use it as a coping strategy for labour.

This is one of the spaces you will come to in Harmony Suite if you are coming in for an Induction of Labour. There is mood lighting, a space to rest and be monitored and birthing balls available. There is an shared bathroom based within the Harmony Suite. It has been purposely built within our Delivery Suite so you have quick access to be transferred or reviewed by our Obstetric Doctors if needed.


